Chinese Journal of Tissue Engineering Research ›› 2015, Vol. 19 ›› Issue (4): 543-547.doi: 10.3969/j.issn.2095-4344.2015.04.009
Previous Articles Next Articles
Modified transmultifidus approach and posterior central approach of vertebrae pedicle screws in the treatment of thoracolumbar vertebral fractures: vertebral stability and related indexes
Hu Zheng-xia, Li Kai-nan, He Zhi-yong
- Department of Orthopedics, Affiliated Hospital of Chengdu University, Chengdu 610081, Sichuan Province, China
-
Revised:2014-12-22Online:2015-01-22Published:2015-01-22 -
Contact:Li Kai-nan, Chief physician, Master’s supervisor, Department of Orthopedics, Affiliated Hospital of Chengdu University, Chengdu 610081, Sichuan Province, China -
About author:Hu Zheng-xia, Master, Physician, Department of Orthopedics, Affiliated Hospital of Chengdu University, Chengdu 610081, Sichuan Province, China -
Supported by:the National Natural Science Foundation of China, No. 81171753
CLC Number:
Cite this article
Hu Zheng-xia, Li Kai-nan, He Zhi-yong. Modified transmultifidus approach and posterior central approach of vertebrae pedicle screws in the treatment of thoracolumbar vertebral fractures: vertebral stability and related indexes[J]. Chinese Journal of Tissue Engineering Research, 2015, 19(4): 543-547.
share this article
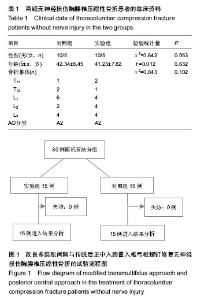
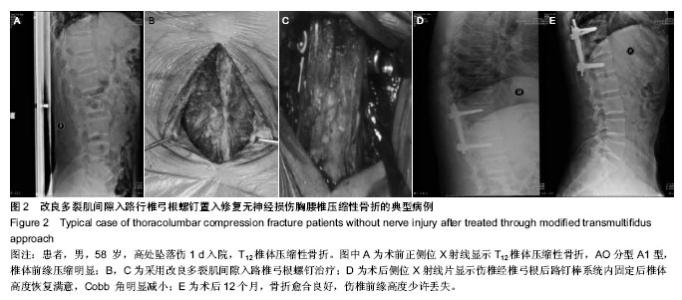
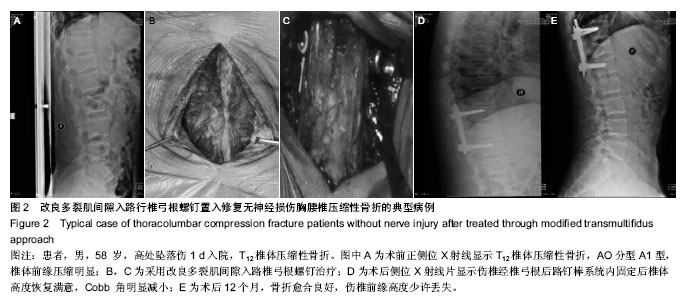
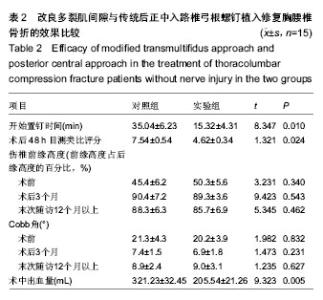
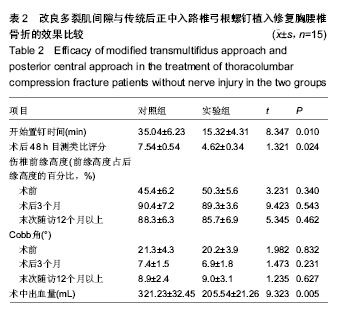
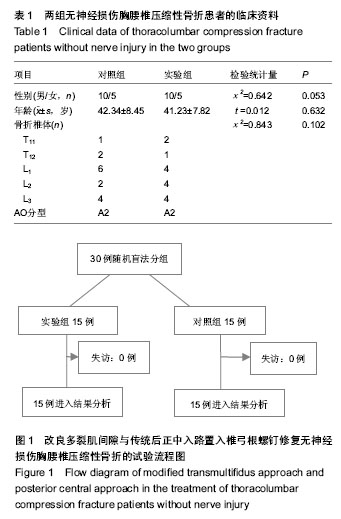
2.1 参与者数量分析及临床信息 所有无神经损伤胸腰椎压缩性骨折患者均获随访,时间均超过12个月。两组无神经损伤胸腰椎压缩性骨折患者在性别、年龄、骨折椎体方面差异无显著性意义(表1)。试验流程见图1。 2.2 两组治疗效果比较 改良肌间隙入路较传统后正中入路治疗无神经损伤胸腰椎压缩性骨折不仅可以明显缩短置钉时间,进而缩短手术时间,而且可以减少术中出血量,术后患者的目测类比评分明显优于传统后正中入路组(P < 0.05);但两组患者伤椎前缘高度恢复及Cobb角的改变差异无显著性意义(P > 0.05),见表2。 2.3 不良反应及并发症 所有无神经损伤胸腰椎压缩性骨折患者术后伤口均未出现感染,脂肪液化等,均为甲级愈合,术后12d左右伤口拆线。 2.4 典型病例 患者,男,58 岁,高处坠落伤1 d后入院,T12椎体压缩性骨折,AO分型A1型,椎体前缘压缩明显;采用改良多裂肌间隙入路椎弓根螺钉置入内固定,X射线显示伤椎椎体高度恢复满意,Cobb角明显减小;术后12个月复查,骨折愈合良好,伤椎前缘高度少许丢失(图2)。"
| [1] Weber BR, Grob D, Dvorák J, et al. Posterior surgical approach to the lumbar spine and its effect on the multifidus muscle. Spine (Phila Pa 1976). 1997;22(15):1765-1772.
[2] Kim CW. Scientific basis of minimally invasive spine surgery: prevention of multifidus muscle injury during posterior lumbar surgery. Spine (Phila Pa 1976). 2010;35 (26 Suppl): S281-286.
[3] Hoh DJ, Wang MY, Ritland SL. Anatomic features of the paramedian muscle-splitting approaches to the lumbar spine. Neurosurgery. 2010;66(3 Suppl Operative):13-25.
[4] Hu ZJ, Fang XQ, Fan SW. Iatrogenic injury to the erector spinae during posterior lumbar spine surgery: underlying anatomical considerations, preventable root causes, and surgical tips and tricks. Eur J Orthop Surg Traumatol. 2014; 24(2):127-135.
[5] Kalimo H, Rantanen J, Viljanen T, et al. Lumbar muscles: structure and function. Ann Med. 1989;21(5):353-359.
[6] Zanoli G. Outcome assessment in lumbar spine surgery. Acta Orthop Suppl. 2005;76(318):5-47.
[7] 宓士军,刘长林,郑智慧,等.经皮椎弓根内固定联合椎体成形术治疗骨质疏松椎体压缩骨折[J].中国骨与关节损伤杂志,2011, 26(1): 59-60.
[8] Wiltse LL, Spencer CW. New uses and refinements of the paraspinal approach to the lumbar spine. Spine (Phila Pa 1976). 1988;13(6):696-706.
[9] McCulloch JA, Weiner BK. Microsurgery in the lumbar intertransverse interval. Instr Course Lect. 2002;51:233-241.
[10] Grifka J, Witte H, Faustmann P, et al. Surgical approach in lumbar intervertebral disk displacement. Topographical principles and characteristics. Orthopade. 1999;28(7): 572-578.
[11] Palmer DK, Allen JL, Williams PA, et al. Multilevel magnetic resonance imaging analysis of multifidus-longissimus cleavage planes in the lumbar spine and potential clinical applications to Wiltse's paraspinal approach. Spine (Phila Pa 1976). 2011;36(16):1263-1267.
[12] Edwards CC 2nd, Bridwell KH, Patel A, et al. Long adult deformity fusions to L5 and the sacrum. A matched cohort analysis. Spine (Phila Pa 1976). 2004;29(18):1996-2005.
[13] Hebert JJ, Marcus RL, Koppenhaver SL, et al. Postoperative rehabilitation following lumbar discectomy with quantification of trunk muscle morphology and function:a case report and review of the literature.J Orthop Sports Phys Ther. 2010; 40(7):402-412.
[14] 罗肖,陈敬忠,张怀学.经皮球囊扩充椎体成型术治疗无神经损伤胸腰椎骨折的临床观察[J].中国现代医药杂志,2013,15(7): 21-23.
[15] Fukui M, Chiba K, Kawakami M, et al. Japanese Orthopaedic Association Back Pain Evaluation Questionnaire. Part 2. Verification of its reliability : The Subcommittee on Low Back Pain and Cervical Myelopathy Evaluation of the Clinical Outcome Committee of the Japanese Orthopaedic Association. J Orthop Sci. 2007;12(6):526-532.
[16] Longo UG, Loppini M, Denaro L, et al. Rating scales for low back pain. Br Med Bull. 2010;94:81-144.
[17] Müller U, Duetz MS, Roeder C, et al. Condition-specific outcome measures for low back pain. Part I: validation. Eur Spine J. 2004;13(4):301-313.
[18] Müller U, Roeder C, Dubs L, et al. Condition-specific outcome measures for low back pain. Part II: scale construction. Eur Spine J. 2004;13(4):314-324.
[19] Kim DY, Lee SH, Chung SK, et al. Comparison of multifidus muscle atrophy and trunk extension muscle strength: percutaneous versus open pedicle screw fixation. Spine (Phila Pa 1976). 2005;30(1):123-129.
[20] Mobbs RJ, Sivabalan P, Li J. Technique, challenges and indications for percutaneous pedicle screw fixation. J Clin Neurosci. 2011;18(6):741-749.
[21] Weinstein JN, Rydevik BL, Rauschning W. Anatomic and technical considerations of pedicle screw fixation. Clin Orthop Relat Res. 1992;(284):34-46.
[22] Palmisani M, Gasbarrini A, Brodano GB, et al. Minimally invasive percutaneous fixation in the treatment of thoracic and lumbar spine fractures. Eur Spine J. 2009;18 Suppl 1:71-74.
[23] Parker JW, Lane JR, Karaikovic EE, et al. Successful short-segment instrumentation and fusion for thoracolumbar spine fractures: a consecutive 41/2-year series. Spine (Phila Pa 1976). 2000;25(9):1157-1170.
[24] Knop C, Blauth M, Bastian L, et al. Fractures of the thoracolumbar spine. Late results of dorsal instrumentation and its consequences. Unfallchirurg. 1997;100(8):630-639.
[25] Liu Y, Yin Q, Gu S, et al. Research progress of stress fracture of lumbar pedicle. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2013;27(2):240-242.
[26] Rutherford EE, Tarplett LJ, Davies EM, et al. Lumbar spine fusion and stabilization: hardware, techniques, and imaging appearances. Radiographics. 2007;27(6):1737-1749.
[27] Ha AS, Petscavage-Thomas JM. Imaging of current spinal hardware: lumbar spine. AJR Am J Roentgenol. 2014;203(3): 573-581.
[28] Spena G, Panciani PP, Costi E, et al. Minimally invasive surgery for thoracic and lumbar spinal fractures: rationale for treatment. J Neurosurg Sci. 2014;58(2 Suppl 1):23-27.
[29] Wild MH, Glees M, Plieschnegger C, et al. Five-year follow-up examination after purely minimally invasive posterior stabilization of thoracolumbar fractures: a comparison of minimally invasive percutaneously and conventionally open treated patients. Arch Orthop Trauma Surg. 2007;127(5): 335-343.
[30] Knop C, Bastian L, Lange U, et al. Transpedicular fusion of the thoraco-lumbar junction. Clinical, radiographic and CT results. Orthopade. 1999;28(8):703-713.
[31] Korovessis P, Repantis T, Iliopoulos P, et al. Beneficial influence of titanium mesh cage on infection healing and spinal reconstruction in hematogenous septic spondylitis: a retrospective analysis of surgical outcome of twenty-five consecutive cases and review of literature. Spine (Phila Pa 1976). 2008;33(21):E759-767.
[32] Hakalo J, Wroński J. Complications of a transpedicular stabilization of thoraco-lumbar burst fractures. Neurol Neurochir Pol. 2006;40(2):134-139.
[33] Pizanis A, Mutschler W. Dorsal stabilization of fractures of the thoracic and lumbar spine by external fixator--technique and outcome. Zentralbl Chir. 1998;123(8):936-943.
[34] Bellabarba C, Fisher C, Chapman JR, et al. Does early fracture fixation of thoracolumbar spine fractures decrease morbidity or mortality? Spine (Phila Pa 1976). 2010;35(9 Suppl):S138-145.
[35] Court C, Vincent C. Percutaneous fixation of thoracolumbar fractures: current concepts. Orthop Traumatol Surg Res. 2012;98(8):900-909.
[36] Peng J, Xu J. Research progress in surgical treatment of thoracolumbar fracture. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2009;23(12):1506-1509.
[37] Amini A, Beisse R, Schmidt MH. Thoracoscopic spine surgery for decompression and stabilization of the anterolateral thoracolumbar spine. Neurosurg Focus. 2005;19(6):E4.
[38] Rampersaud YR, Annand N, Dekutoski MB. Use of minimally invasive surgical techniques in the management of thoracolumbar trauma: current concepts. Spine (Phila Pa 1976). 2006;31(11 Suppl):S96-102; discussion S104.
[39] Vaccaro AR. Combined anterior and posterior surgery for fractures of the thoracolumbar spine. Instr Course Lect. 1999; 48:443-449.
[40] Oner FC, Dhert WJ, Verlaan JJ. Less invasive anterior column reconstruction in thoracolumbar fractures. Injury. 2005; 36 Suppl 2:B82-89.
[41] Kim DH, Jaikumar S, Kam AC. Minimally invasive spine instrumentation. Neurosurgery. 2002;51(5 Suppl):S15-25.
[42] 胡庆丰,范顺武,潘浩,等.肌间隙入路椎弓根钉固定结合椎体成形术治疗胸腰椎骨折[J].中国中西医结合外科杂志,2010, 16(1): 5-9.
[43] 汪学军,李开南,母建松,等.椎间盘镜下椎弓根螺钉内固定治疗胸腰椎骨折[J].中国矫形外科杂志,2007,15(4):316-317.
[44] 张强,纪玉清,胡樵,等.胸腰椎骨折后路微创器械的设计及临床应用[J].中华创伤骨科杂志,2010,1212(7):605-608.
[45] 王景续,杨冬,郭勇,等.经椎弓根植骨技术治疗胸腰椎骨折[J].中国临床医学,2007,14(2):238-239.
[46] 国家中医药管理局.中医病症诊断疗效标准[M].南京:南京大学出版社,1994:176.
[47] 陈宣煌,许卫红,胡建伟,等.小切口椎旁肌间隙入路和传统开放式入路腰椎后路融合术的比较[J].脊柱外科杂志,2012,4(2): 101-104.
[48] 侯树勋.现代创伤骨科学[M].北京:人民军医出版社,2002: 950-988.
[49] 那孟奇. Wiltse肌间隙入路与传统后正中入路在治疗胸腰段骨折的比较研究[J].右江民族医学院院报,2011,33(2):145-147.
[50] 邓万祥,赵胡瑞,刘华,等.经伤椎置钉治疗胸腰椎骨折的临床研究[J].中国骨伤,2011,24(7):541-543.
[51] Vialle R, Wicart P, Drain O, et al. The Wiltse paraspinal approach to the lumbar spine revisited: an anatomic study. Clin Orthop Relat Res. 2006;445:175-180.
[52] Gazzeri R, Tamorri M, Galarza M, et al. Balloon-assisted endoscopic retroperitoneal gasless approach (BERG) for lumbar interbody fusion: is it a valid alternative to the laparoscopic approach? Minim Invasive Neurosurg. 2007; 50(3):150-154.
[53] MacDonald DA, Moseley GL, Hodges PW. The lumbar multifidus: does the evidence support clinical beliefs? Man Ther. 2006;11(4):254-263.
[54] Warren A, Prasad V, Thomas M. Pre-operative planning when using the Wiltse approach to the lumbar spine. Ann R Coll Surg Engl. 2010;92(1):74-75. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [3] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [4] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [5] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [6] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [7] | Wang Debin, Bi Zhenggang. Related problems in anatomy mechanics, injury characteristics, fixed repair and three-dimensional technology application for olecranon fracture-dislocations [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1446-1451. |
| [8] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [9] | Xu Yulin, Shen Shi, Zhuo Naiqiang, Yang Huilin, Yang Chao, Li Yang, Zhao Heng, Zhao Lu. Biomechanical comparison of three different plate fixation methods for acetabular posterior column fractures in standing and sitting positions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 826-830. |
| [10] | Cai Qunbin, Zou Xia, Hu Jiantao, Chen Xinmin, Zheng Liqin, Huang Peizhen, Lin Ziling, Jiang Ziwei. Relationship between tip-apex distance and stability of intertrochanteric femoral fractures with proximal femoral anti-rotation nail: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 831-836. |
| [11] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [12] | He Li, Tian Wei, Xu Song, Zhao Xiaoyu, Miao Jun, Jia Jian. Factors influencing the efficacy of lumbopelvic internal fixation in the treatment of traumatic spinopelvic dissociation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 884-889. |
| [13] | Yang Weiqiang, Ding Tong, Yang Weike, Jiang Zhengang. Combined variable stress plate internal fixation affects changes of bone histiocyte function and bone mineral density at the fractured end of goat femur [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 890-894. |
| [14] | Zhang Lei, Ma Li, Fu Shijie, Zhou Xin, Yu Lin, Guo Xiaoguang. Arthroscopic treatment of greater tuberosity avulsion fractures with anterior shoulder dislocation using the double-row suture anchor technique [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 895-900. |
| [15] | Zhang Jing, Wang Bin, Lü Xin. Application of anatomic intramedullary nail in tubular bone fractures of limbs: stronger holding force and anti-rotation ability [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 917-922. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||